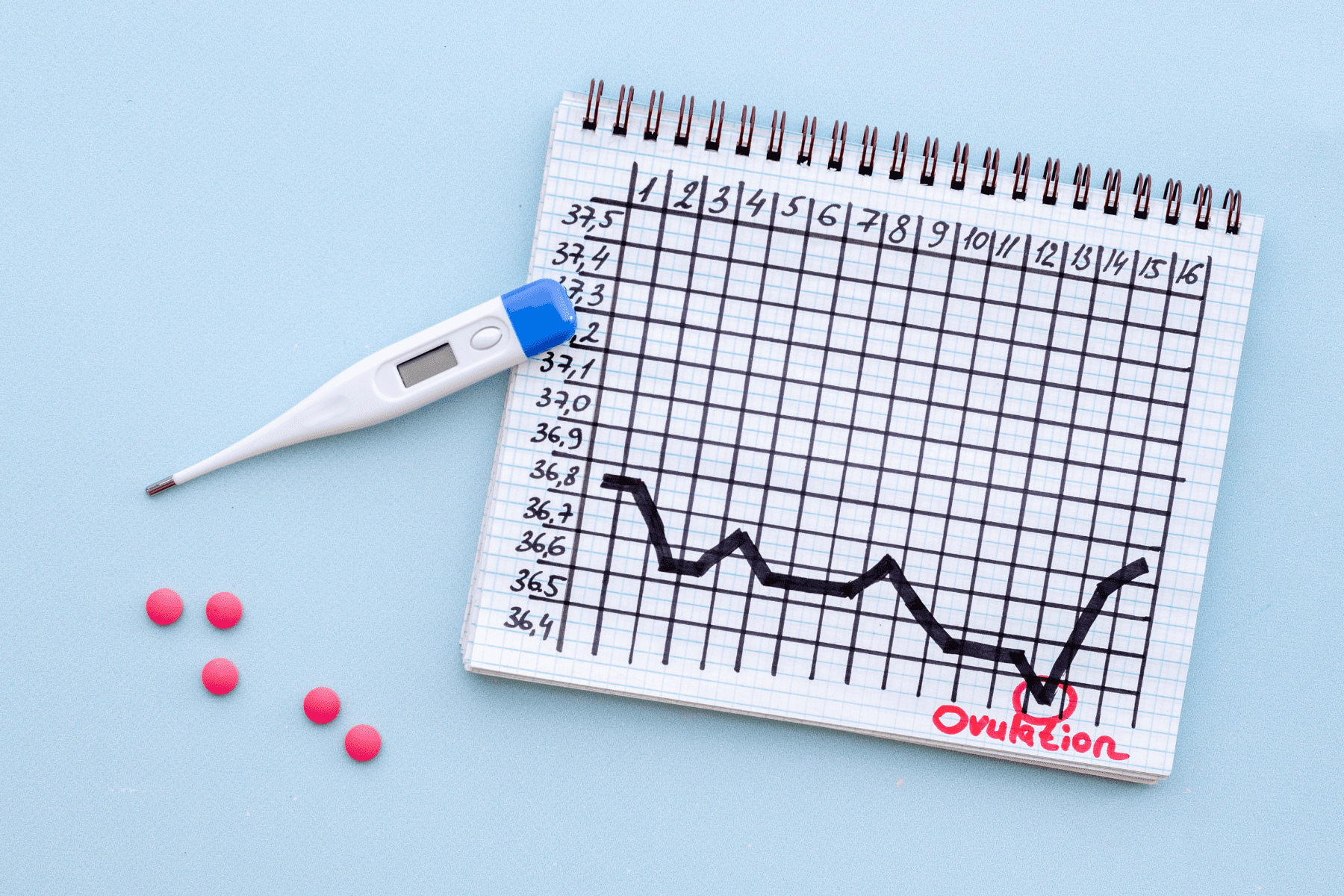
Every month – roughly 7 to 10 days after menstruation – an egg is released from an ovary in a process called ovulation. As the egg travels down the fallopian tube in the hopes of being fertilized, it will survive for up to 24 hours before the “conception window” closes until the next cycle.
The body sends several ovulation signals, but tuning into the signs can take a bit of practice. Some signs are easy to notice, while others require more dedication. Once you’ve learned them, you’ll be a pro at reading your body! And if you are tracking your cycles and think ovulation issues are affecting your ability to get pregnant, schedule a consult with a fertility specialist.
7 signs of ovulation
3 signs indicating you may not be ovulating
If you have been tracking your cycles and are unsure whether you are ovulating, there are some signs that may indicate potential issues:
If you are concerned about your cycle
Tracking your cycle is an important part of learning about your body and uncovering potential issues. There are many free phone apps – Kindara, Glow, Ovia, Flo – that can help determine the most fertile period. These apps also calculate helpful info such as cycle length and offer a history of all cycles recorded at the touch of your fingertips.
If you are concerned about your cycles, seek the help and evaluation of a doctor. Ovulation issues are the most common cause of infertility challenges and with many patients, ovulation can be restored through medication. Some women are even able to make lifestyle changes and resume ovulation without medication. We are here to help you and wish you the best on your journey!
Medical contribution by Jane Nani, M.D.
Dr. Jane Nani is board certified in Obstetrics and Gynecology and in Reproductive Endocrinology and Infertility (REI), and has been practicing medicine since 1996.